
For nearly two decades, Nyobie Gordon-Ricks lived in a ghost story. The antagonist was her own body; the haunting was a shifting phantasm of symptoms that no one—not her family, and certainly not her doctors—seemed to believe was real.
Before the name “lupus” finally gave shape to her suffering in 2010, Gordon-Ricks had been told she had everything from ringworm to leukemia. Sometimes, she was told she had nothing at all, save for a vivid imagination or a “mental episode.”
“For years, I went to doctors and nobody listened to me,” says the 48-year-old pharmacy technician. “I felt like no one understood and no one believed that there was really something wrong with me.”

A Chameleon in the Clinic
Her grueling odyssey to a diagnosis is a familiar narrative for those living with lupus, an autoimmune disease that effectively turns the body’s defense system against its own healthy tissue. Because the illness is a master of mimicry, its calling cards—migraines, exhaustion, joint swelling, and hair loss—often lead clinicians down the wrong path.
“A big problem is, even in great medical centers, sometimes it takes a lot of time to diagnose,” explains Dr. George Tsokos, a professor at Harvard Medical School and chief of rheumatology at Beth Israel Deaconess Medical Center. Dr. Tsokos, who serves on the Lupus Foundation of America’s Medical-Scientific Advisory Council, warns that the disease is as individual as a fingerprint. “If there are symptoms that are not explained, insist on getting more expert opinions. Find people who can treat early and treat aggressively.”

The Silence of the Living Room Floor
The first tremors of the coming storm appeared when Gordon-Ricks was just 13. Her joints swelled, her back ached, and a telltale rash bloomed across her face. A doctor dismissed it as the mere turbulence of puberty.
A year later, the symptoms turned terrifying: partial paralysis.
“I would go numb from my waist down,” she recalls. Her mother, misinterpreting the teenage girl’s immobility for defiance, thought she was simply trying to skip school. “I would literally lay on our living room floor for hours, waiting for the feeling to come back.”
When an ambulance finally took her to a hospital during a second episode, she wasn’t met with a specialist, but with a stigma. Labeled as having a “mental episode,” she was discharged after two days. The rejection was more painful than the paralysis. “After that, I was like, ‘I’m just not going to tell anybody anything anymore because nobody’s believing me.’”
The Breaking Point
By 2009, Gordon-Ricks was 32, engaged, and planning a wedding. But the ghost was getting louder. A rash spread across her limbs; one dermatologist called it ringworm, while another simply shrugged.
The turning point finally came in May 2010. During a routine visit to her gynecologist, Gordon-Ricks laid out the years of chaos. The resulting bloodwork was a red flag: her platelets and blood cell counts were plummeting. The diagnosis wasn’t immediate—she was shuttled through five more specialists who speculated on leukemia, multiple sclerosis, or rheumatoid arthritis.
On December 11, 2010—five days before her 33rd birthday—the sixth specialist provided the answer: Lupus.
“I’m feeling a little bit of relief because now I know what’s wrong with me,” she says of that moment, “but now I’m scared because I don’t know what this means for me.”

The War Within
The “invisible” nature of lupus became a wall between Nyobie and the world. Her fiancé’s aunt had the disease and “seemed fine,” a common refrain that Nyobie had to dismantle.
“I said, ‘From what I understand, a person can look fine but still be sick. Right now, I know physically I look good. But I feel like crap.’”
The transition from “healthy” mother to a patient in crisis was brutal. A woman who used to wrestle with her children now found a simple hug agonizing. She lived in the short, exhausting distance between her bed and the bathroom. She was plagued by “brain fog” and “thumping” headaches that felt like a heartbeat inside her skull.
A full-body scan eventually revealed the terrifying extent of the damage: Lupus cerebritis.
“He said, ‘You have inflammation from your brain to your toes. There is some type of swelling in every single part of your body,’” she remembers. “I was scared for my life. Can I die from this?”
Remission and Resilience
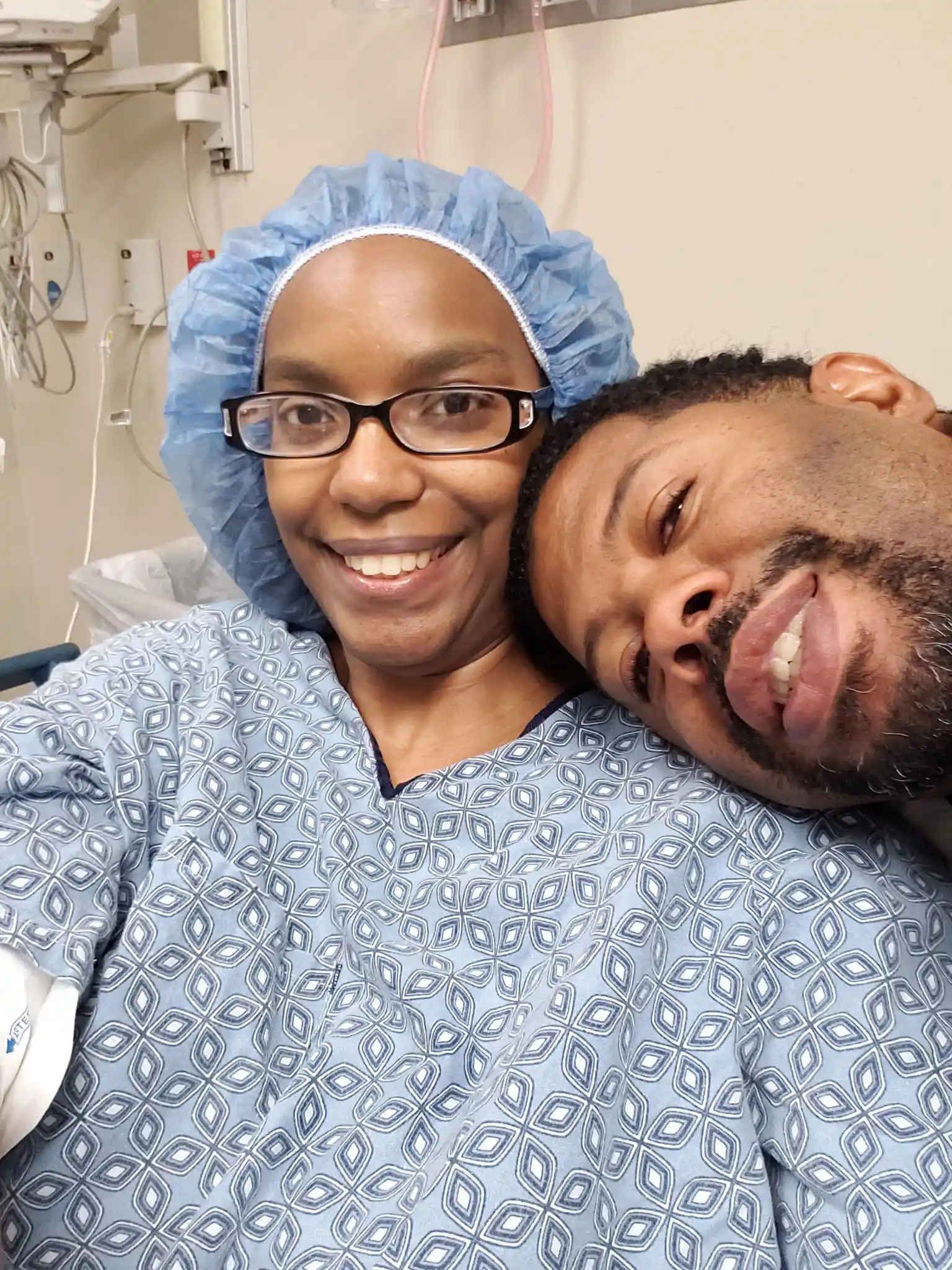
The road back required 12 rounds of chemotherapy beginning in 2012. When she returned to the gynecologist who first believed her, the professional relationship dissolved into a moment of pure human connection. “I told her, ‘You literally saved my life… I don’t think I would be here if you didn’t listen to me.’ She just hugged me and I cried like a baby.”
Life continued despite the scars. She married her fiancé in 2014, a man she describes as her “big support,” who learned to see the pain she tried to hide. Though the disease necessitated a full hysterectomy in 2018, her lupus nephritis moved into remission the year prior.
Today, Nyobie Gordon-Ricks is no longer a silent victim on a living room floor. As an ambassador for the Lupus Foundation of America and the founder of the Arizona Butterfly Warriors, she has turned her nineteen years of silence into a megaphone for others.
“The biggest advice I can give is: Never give up. Learn how to be an advocate for yourself,” she says. “If you know in your heart something’s wrong with you, you need to keep going until you get the answers that you deserve. A lupus diagnosis is not a death sentence. We can survive this.”